We are Launching Live Zoom Classes for 9th and 10th-grade Students. The first batch is from 7th April 2025. Register for a Free demo class.
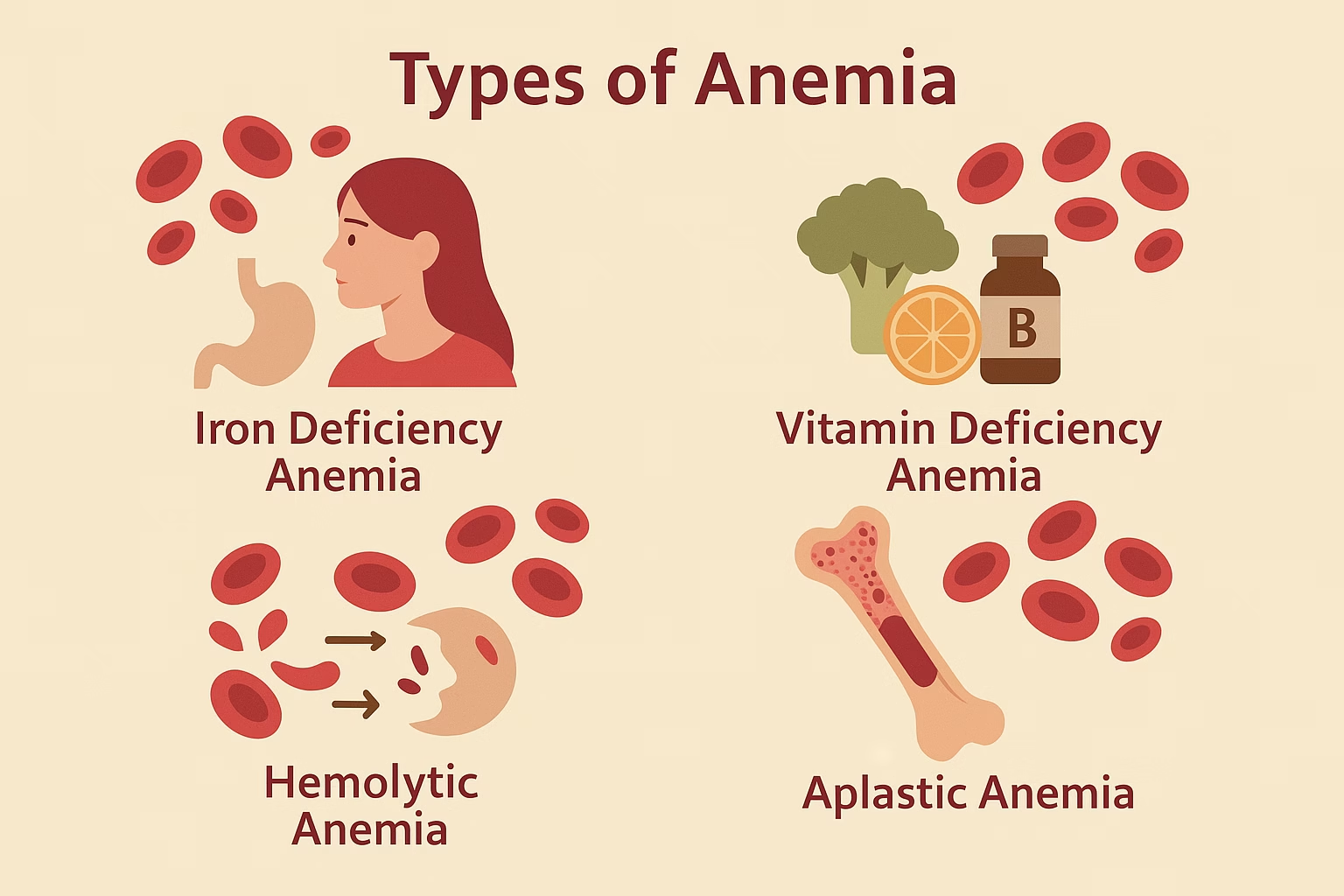
Understanding Anemia: Types, Causes, Symptoms, and Treatment
Introduction
Anemia is one of the most common blood disorders, affecting over 1.6 billion people worldwide, with women, children, and the elderly being the most vulnerable populations 4. It occurs when the body lacks enough healthy red blood cells (RBCs) or hemoglobin, the iron-rich protein that carries oxygen to tissues. This deficiency leads to symptoms like fatigue, weakness, shortness of breath, and dizziness.
Anemia is not a disease itself but rather a symptom of underlying conditions, ranging from nutritional deficiencies to chronic diseases and genetic disorders. Proper diagnosis and treatment depend on identifying the specific type of anemia.
This article explores the different types of anemia, their causes, symptoms, diagnostic methods, and treatments, providing a comprehensive understanding of this widespread condition.
1. Classification of Anemia
Anemia can be classified based on:
- Red Blood Cell (RBC) Size (microcytic, normocytic, macrocytic) 7
- Underlying Cause (nutritional deficiency, blood loss, genetic disorders) 1
- Mechanism (decreased production vs. increased destruction of RBCs) 6
The most common classification is by Mean Corpuscular Volume (MCV), which measures RBC size:
| Type | MCV Range | Common Causes |
|---|---|---|
| Microcytic | <80 fL | Iron deficiency, thalassemia, chronic disease |
| Normocytic | 80–100 fL | Chronic disease, hemolysis, bone marrow disorders |
| Macrocytic | >100 fL | B12/folate deficiency, liver disease, alcoholism |
Let’s examine each type in detail.
2. Microcytic Anemia (Small RBCs)
Microcytic anemia occurs when RBCs are smaller than normal, usually due to insufficient hemoglobin production. The main causes include:
A. Iron-Deficiency Anemia (Most Common Type)
- Causes:
- Blood loss (heavy menstruation, GI bleeding)
- Poor dietary iron intake
- Malabsorption (celiac disease, gastric bypass) 16
- Symptoms:
- Fatigue, pale skin, brittle nails
- Pica (craving non-food items like ice or dirt) 6
- Treatment:
- Iron supplements (ferrous sulfate)
- Dietary changes (red meat, leafy greens, fortified cereals) 8
B. Thalassemia (Genetic Disorder)
- Inherited condition causing abnormal hemoglobin production 9.
- Symptoms:
- Mild to severe anemia, jaundice, bone deformities (in severe cases).
- Treatment:
- Blood transfusions, folic acid supplements, bone marrow transplant (in severe cases) 3.
C. Anemia of Chronic Disease (ACD)
- Seen in chronic infections (HIV, TB), autoimmune diseases (rheumatoid arthritis), and cancer 1.
- Mechanism: Inflammation disrupts iron metabolism, reducing RBC production.
- Treatment: Managing the underlying condition, sometimes iron or erythropoietin therapy 6.
3. Normocytic Anemia (Normal-Sized RBCs)
In normocytic anemia, RBCs are normal in size but too few in number. Causes include:
A. Hemolytic Anemia (Premature RBC Destruction)
- Causes:
- Autoimmune disorders (immune system attacks RBCs)
- Infections (malaria)
- Genetic disorders (sickle cell disease, G6PD deficiency) 6.
- Symptoms:
- Jaundice, dark urine (from hemoglobin breakdown).
- Treatment:
- Immunosuppressants, blood transfusions, treating infections 3.
B. Aplastic Anemia (Bone Marrow Failure)
- Causes:
- Toxins, radiation, chemotherapy, viral infections (e.g., hepatitis) 8.
- Symptoms:
- Fatigue, frequent infections (low WBCs), easy bruising (low platelets).
- Treatment:
- Bone marrow transplant (curative), immunosuppressants, blood transfusions 3.
C. Blood Loss Anemia
- Acute (trauma, surgery) or chronic (GI bleeding, heavy periods) 1.
- Treatment:
- Blood transfusion (if severe), iron supplementation, stopping the source of bleeding.
4. Macrocytic Anemia (Large RBCs)
Macrocytic anemia occurs when RBCs are larger than normal, often due to DNA synthesis issues.
A. Megaloblastic Anemia (B12/Folate Deficiency)
- Causes:
- Vitamin B12 deficiency (pernicious anemia, vegan diet)
- Folate deficiency (poor diet, alcoholism, pregnancy) 6.
- Symptoms:
- Fatigue, neurological issues (numbness, balance problems in B12 deficiency).
- Treatment:
- B12 injections (if absorption issue), oral folate supplements 9.
B. Non-Megaloblastic Macrocytic Anemia
- Causes:
- Liver disease, alcoholism, hypothyroidism, myelodysplastic syndrome (MDS) 7.
- Treatment:
- Managing underlying conditions (e.g., alcohol cessation, thyroid hormone replacement).
5. Diagnosis of Anemia
Diagnosis involves:
- Complete Blood Count (CBC) – Checks hemoglobin, RBC count, MCV 1.
- Peripheral Blood Smear – Examines RBC shape/size.
- Iron Studies – Serum ferritin, iron, TIBC (for iron deficiency).
- Vitamin B12/Folate Levels – For macrocytic anemia.
- Reticulocyte Count – Determines if bone marrow is producing enough RBCs 7.
6. Treatment & Prevention
A. Nutritional Anemias (Iron, B12, Folate)
- Iron-rich foods: Red meat, spinach, lentils.
- B12 sources: Meat, eggs, dairy (or supplements for vegans).
- Folate sources: Leafy greens, citrus fruits, beans 8.
B. Chronic Disease & Genetic Anemias
- Erythropoietin (EPO) injections (for kidney disease).
- Blood transfusions (severe thalassemia, sickle cell).
- Bone marrow transplant (for aplastic anemia, sickle cell) 3.
C. Preventive Measures
- Balanced diet (iron, vitamins).
- Screening (pregnant women, chronic disease patients).
- Malaria prevention in endemic areas 4.
7. Global Impact & WHO Initiatives
- 40% of children under 5 and 30% of women worldwide suffer from anemia 4.
- WHO’s 2025 Goal: Reduce anemia in women by 50% through iron supplementation, malaria control, and nutrition programs 2.
Conclusion
Anemia is a multifaceted condition with varying causes, from simple iron deficiency to complex genetic disorders. Early diagnosis and targeted treatment (dietary changes, supplements, or advanced therapies) can significantly improve quality of life. Public health efforts, including nutritional education and disease prevention, are crucial in reducing its global burden.
If you experience persistent fatigue, dizziness, or pallor, consult a doctor—anemia may be an early warning sign of a deeper health issue.
References
- StatPearls, NCBI – Anemia Classification & Pathophysiology
- WHO – Global Nutrition Targets 2025
- American Society of Hematology – Anemia Overview
- WHO Fact Sheet – Anaemia
- Healthline – Types & Symptoms of Anemia
- StatPearls – MCV & RDW Classification
- Regional Cancer Care – Anemia Treatments
- Healthline – Microcytic, Normocytic, Macrocytic Anemia
